We are investigating how oral health can affect the rest of the body, by studying associations with other health conditions like cardiovascular disease and dementia
Patients who attend emergency departments following a heart attack or stroke often have a higher presence of severe gum disease. We know that inflammation induced by gum disease can increase overall body inflammation and affect the heart and brain, but it is not yet known how influential this effect is. Our researchers are working with NHS colleagues to investigate to what extent gum diseases impact other conditions, and build an exemplar for integrated oral and systemic health care.
Explore our key areas of work by expanding the sections below:
Mapping the co-morbidities associated with gum diseases
We analysed health data for 3,700 patients with gum diseases, using data from the National Health and Nutrition Examination Survey (NHANES) in the USA. The study confirmed previous assumptions that particular health conditions are common in people with gum diseases: cardiovascular disease, cancer, dementia, diabetes and high blood pressure (hypertension). The team used ‘hypergraphs’, a form of artificial intelligence network analysis, to reveal clusters of these diseases that often occur together alongside gum diseases, and to identify which conditions in each cluster may be most influential on the development of others. The full paper is available in Journal of Dental Research: Systemic Multimorbidity Cluster in People with Periodontitis.

Key findings
- People with gum disease are more likely to have high blood pressure and obesity together, and these conditions are highly influential to the presence of other diseases in the body.
- Diabetes was most influential for people with more severe gum disease.
- Ethnicity and deprivation affected the clustering of arthritis and obesity more in people with mild gum disease.
- Smoking status and deprivation affected the clustering pattern of diabetes and cancer in people with severe gum disease.
This is the first time hypergraphs have been used to show the associations between oral and systemic disease. As precision medicine moves to the forefront of population health research, the approach could be extremely valuable for understanding how diseases interact.
Seeking a modifiable risk factor for dementia
We are analysing health data to understand how gum diseases and cognitive decline influence each other. Our aim is to find a modifiable risk factor that could prevent dementia, and to promote integrated dental and general health care for patients.
To establish any causal relationship, we are using observational studies to explore the association between gum diseases and dementia, and we are also studying the genetic association between these diseases. We are using data from NHANES in the USA and UK Biobank - these datasets contain information on health conditions and genetics for ~20,000 and ~500,000 patients respectively. Our researchers are looking for common genetic risk factors for gum diseases and are testing whether people with gum diseases are more likely to have dementia or not. We are also using electronic health records to study whether treating dental diseases reduces the risk of dementia.
This work is supported by Alzheimer’s Society.
Preventing cardiovascular disease
We are linking patient record data from dental hospitals and general hospitals in London and Leeds to study whether treatment for oral health can prevent or improve cardiovascular disease. We are working with patient data from:
- St Bartholomew's Hospital and The Royal London Dental Hospital;
- Guy’s Hospital and King’s College London Dental Institute; and
- Leeds Teaching Hospital and Leeds Dental Hospital.
This work is funded by Barts Charity via a grant awarded jointly to CEG and our Queen Mary colleagues in the Institute of Dentistry. Our long-term aim is to bridge the gap between dental and general health across research and patient care.
The healthcare burden of GP dental patient encounters
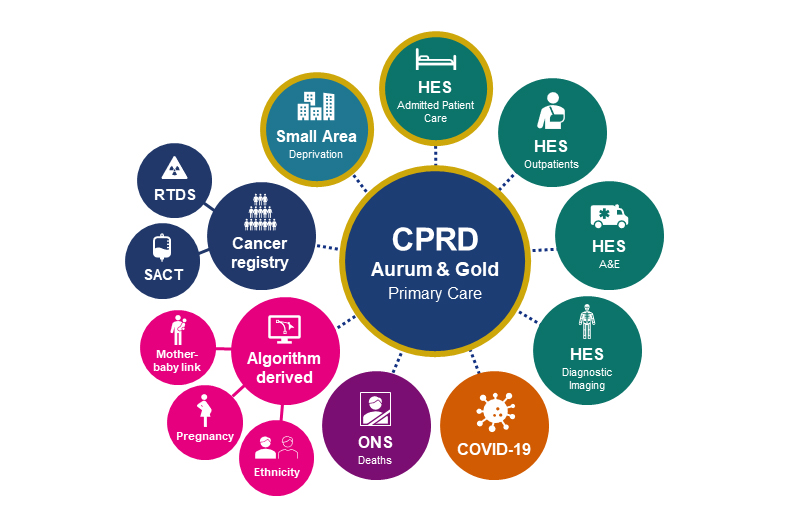
We're studying the numbers and characteristics of people who visit their GP with dental issues. We are using anonymised data on patient age, gender and medical history from CPRD (Clinical Practice Research Datalink) to see who is visiting their GP for dental care, how this changes over time, and how it varies by geographical area.
The results will inform healthcare providers about the wider burden of dental attendances in primary care and could also guide future policy as evidence for better integration of primary care and dental services.